The State of HX
In this paper, Press Ganey thought leaders offer insights and implications from the data, predictions for the future of healthcare, and commentary on which healthcare issues are the most pressing for healthcare leaders to address in 2024.

Building a thriving healthcare workforce
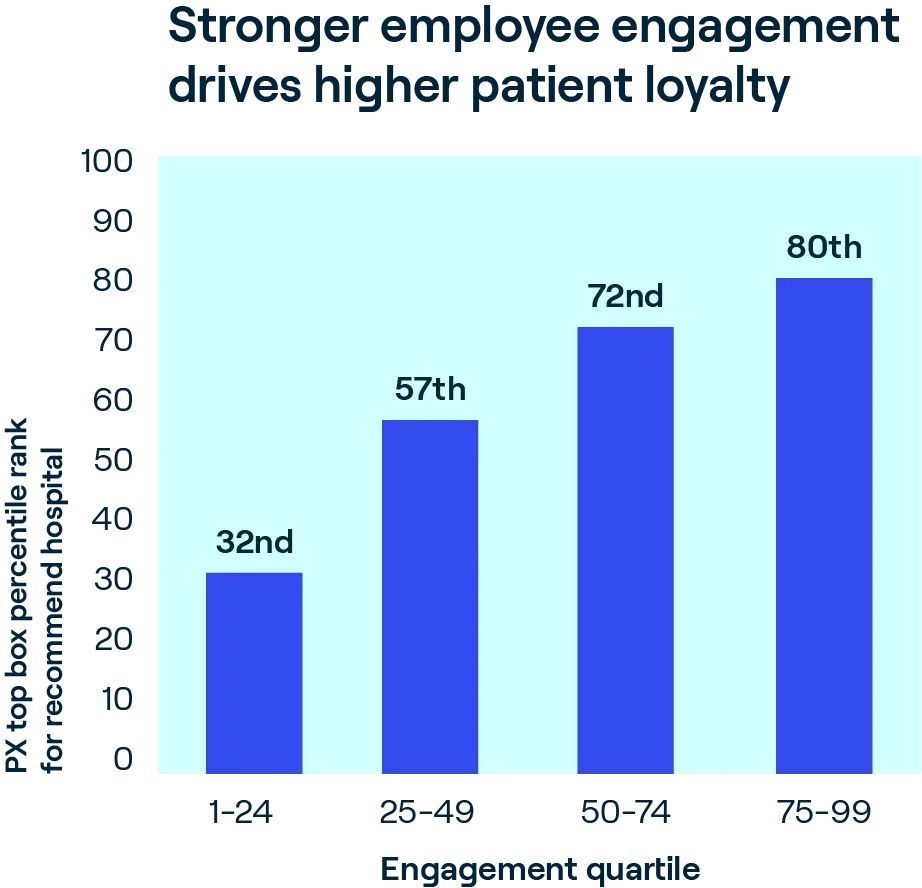
At the heart of great healthcare are the physicians and caregivers dedicated to delivering safe, high-quality, patient-centered outcomes. Efforts to build social capital by nurturing their dedication through engagement strategies create a powerful flywheel effect: Year over year, our data shows the strong association of employee engagement with patient experience, safety, and quality of care.
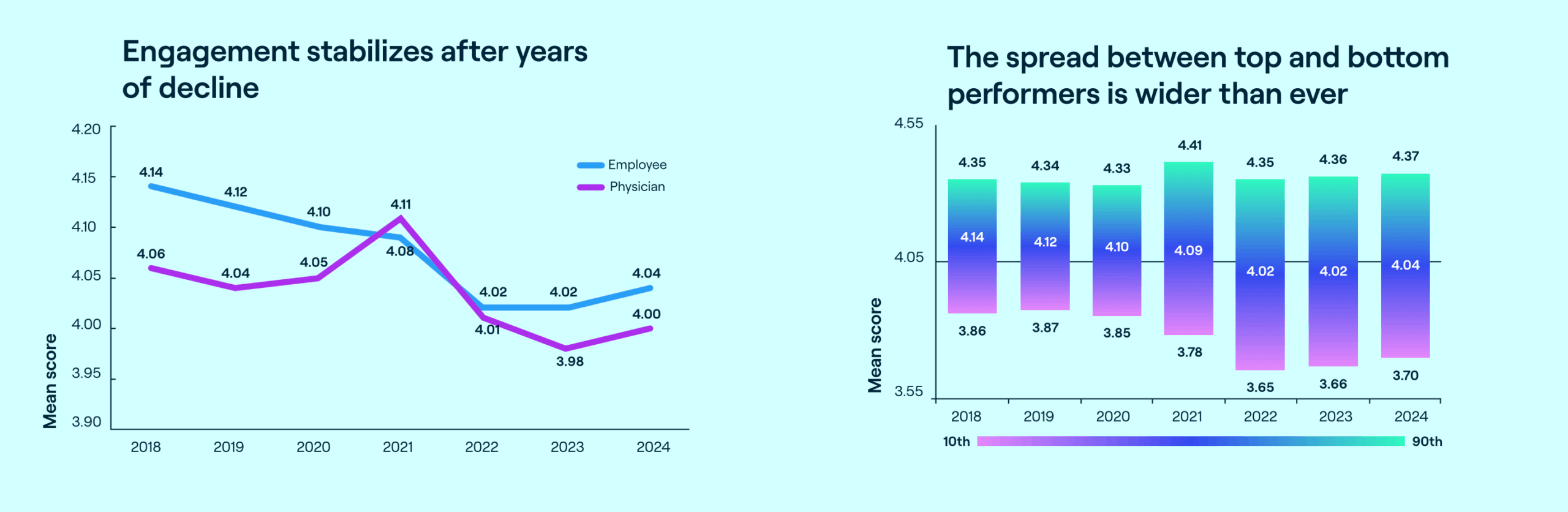
Press Ganey national data, based on responses from 1.4 million employees across 4,000 provider organizations, shows signs that workforce engagement is stabilizing after a multiyear downward trend that began prior to the pandemic. Yet despite these gains, and the inherent rewards of a career in healthcare, many organizations are hard-pressed to attract and retain skilled staff. Addressing workforce issues continues to be the #1 priority among health system CEOs, given current and expected labor shortages.
Underlying the aggregate data is a large gap in engagement between top and bottom performers—a gap that has widened over the last three years. The top decile of performance is now higher than it was before COVID hit, while bottom-decile performance is worse. Important lessons emerge from both ends of the curve—and clear evidence that, with the right approach, it is possible to improve engagement in today’s challenging environment.
Average scores on engagement and intent to remain differ significantly by role, with the lowest scores concentrated among front-line caregivers. Despite modest gains in 2023, nurses, APPs, licensed technical staff, and physicians are consistently at the low end of the engagement curve each year.
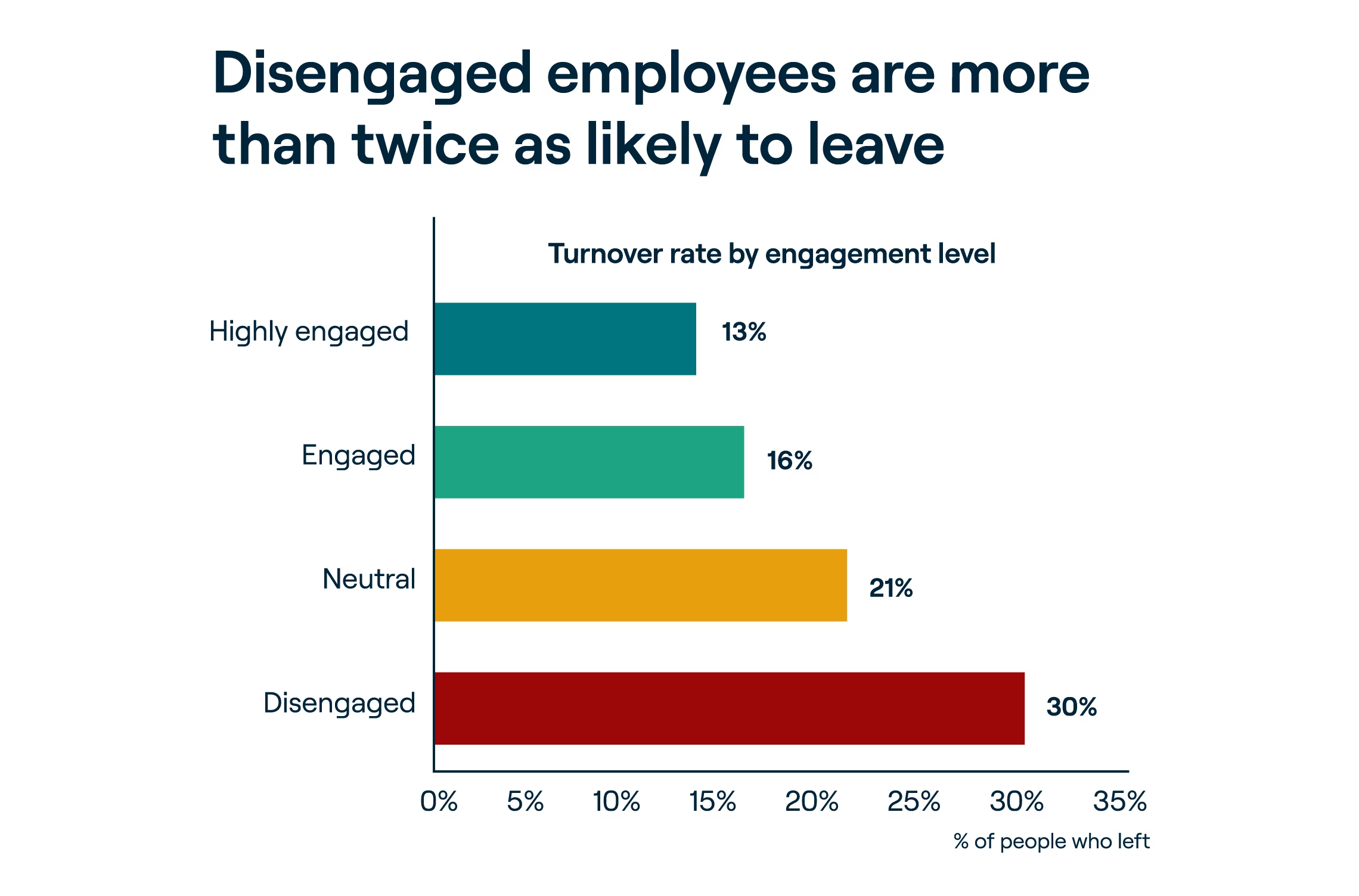
This means the highly skilled people who interact with patients on a daily basis struggle to stay connected to their work and achieve professional fulfillment. And they’re at the highest risk of leaving.
Organizations diagnosing their own opportunities for improving engagement will benefit from looking at performance and performance drivers at different units of analysis—including role, team or work unit, shift, gender, and tenure—to home in on their precise opportunities and next best actions.
Where to focus: Drivers of physician and caregiver engagement
Sustaining high performance on caregiver and provider experience is no accident. A key driver analysis of organizations that have maintained high engagement despite the industry’s macro pressures reveals common strengths, as perceived by their caregivers and providers.
These center on themes of respect, senior management behavior and actions, and commitment to quality and safety—all key facets of trust and social capital. Notably, while compensation and staffing are correlated to engagement, they are not among the top 10 drivers of engagement. Fair pay and adequate staffing are table stakes, but they’re not among the aspects of workforce experience that drive engagement and contribute to the creation of social capital.
Top 10 drivers of employee engagement
Treating employees with respect
Senior management’s actions support the organization’s mission and values
A commitment to quality improvement
Conducting business in an ethical manner
Employees’ perspectives factored into decision-making
The organization’s work climate promotes patient safety
Confidence in senior management’s leadership
Satisfaction with job security
Caring about customers
Caring about employee safety
Safety first
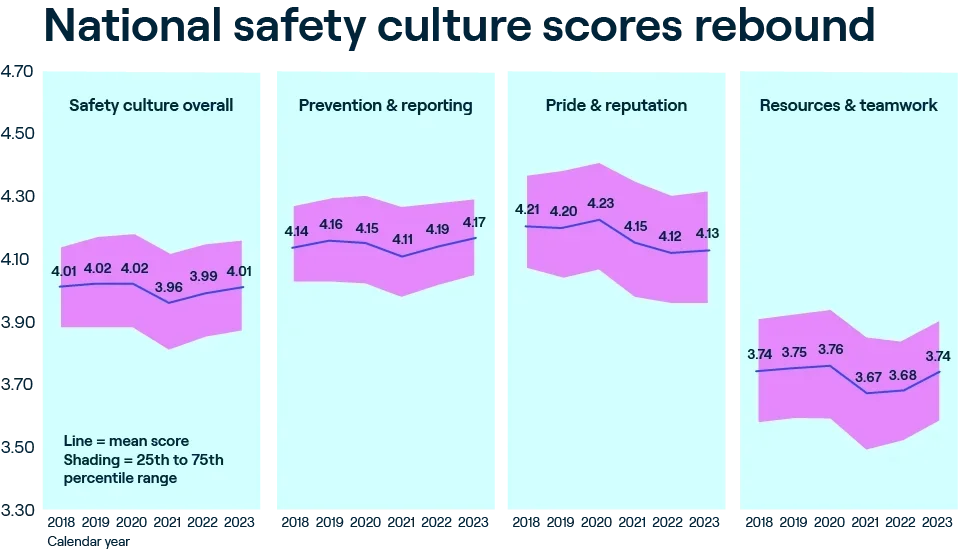
Top-performing healthcare organizations put safety first. This commitment is crucial for patient care as well as for building a sense of pride and motivation among staff. There is a strong positive correlation between safety culture scores and employee engagement—and the magnitude of the correlation has intensified since the start of the pandemic. Annual results from Press Ganey’s safety culture survey, the most widely used in the U.S. with feedback from nearly 1.4 million healthcare workers a year, confirm this pattern.
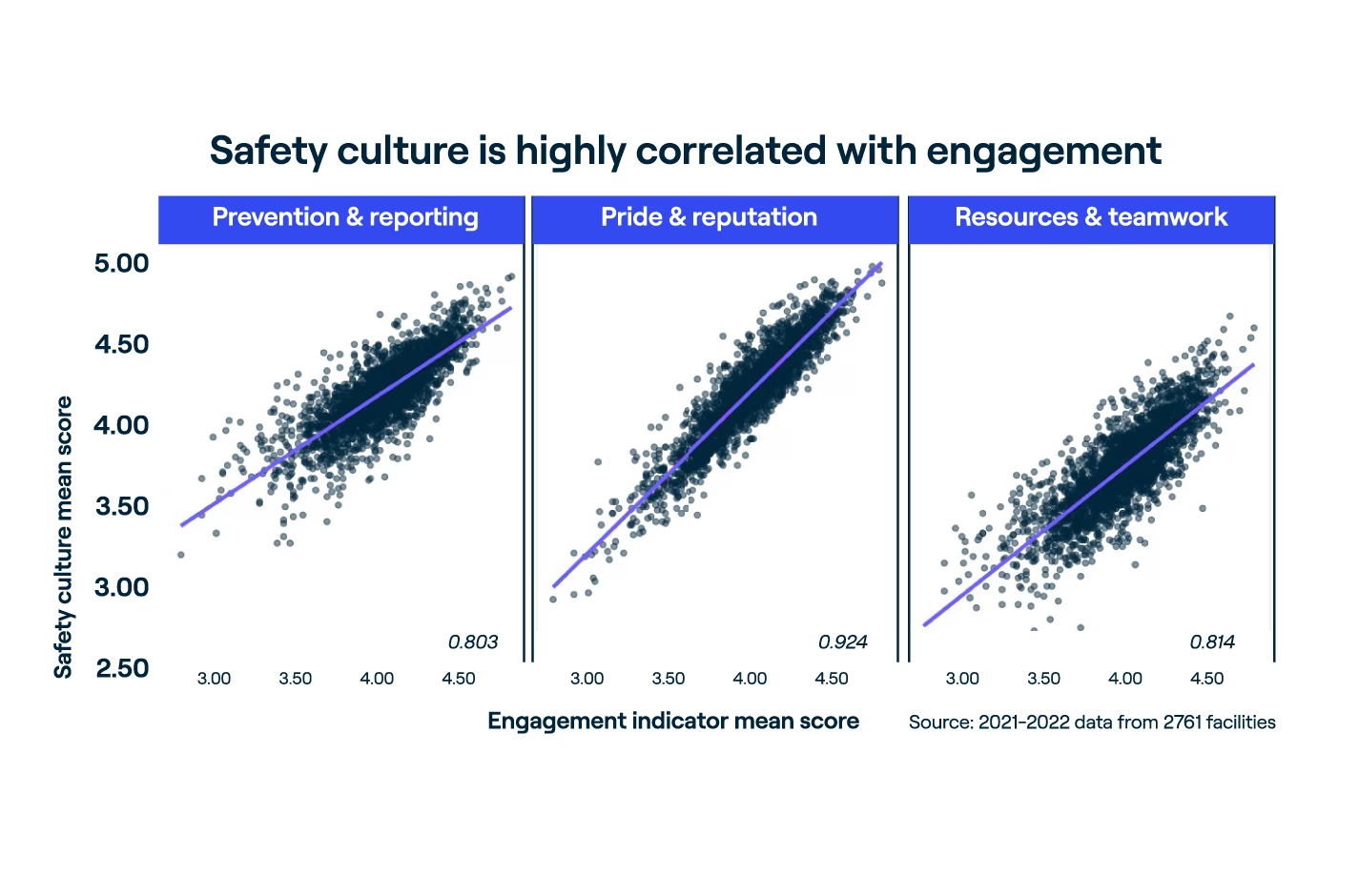
Safety culture is reported as a composite score, but the correlations between engagement and the subscales—resources and teamwork, prevention and reporting, and pride and reputation—illustrate powerful relationships. Simply put, when a healthcare organization prioritizes safety by fostering a culture of safety, its employees are more able to be fully invested in their work.
Prior to the pandemic, national aggregate safety culture scores were on the rise—and safety events were on the decline. But the stress of COVID on the healthcare system eroded national performance across all measures. In 2021, organizations redoubled efforts around safety, and results in 2022 brought gains in the prevention and reporting subscale, followed by gains across all subscales in 2023.
Notably, it is among employees in front-line roles where we saw the greatest improvement in perception on questions related to resources and teamwork and prevention and reporting. Safety culture is a rising tide measure: Organizations that continue to invest in this area will realize gains across patient, caregiver, and business outcomes.
Organizations with the strongest safety cultures have multiple attributes and practices in common. These include highly visible leadership, tiered safety huddles, leader rounding, transparency around issue identification and resolution, and high reliability communication behaviors for leaders, managers, and front-line staff. They also involve front-line staff in improvement initiatives—with the dual benefit of faster improvement cycle time and fostering better engagement.
Drivers of retention
Retaining the skilled people we recruit is a universal priority, yet it’s getting harder to do. An examination of employee census data from health systems and hospitals that survey annually with Press Ganey reveals that between 2022 and 2023, one in five healthcare employees left their organization—a rate that increases to one in four for employees with less than two years’ tenure.
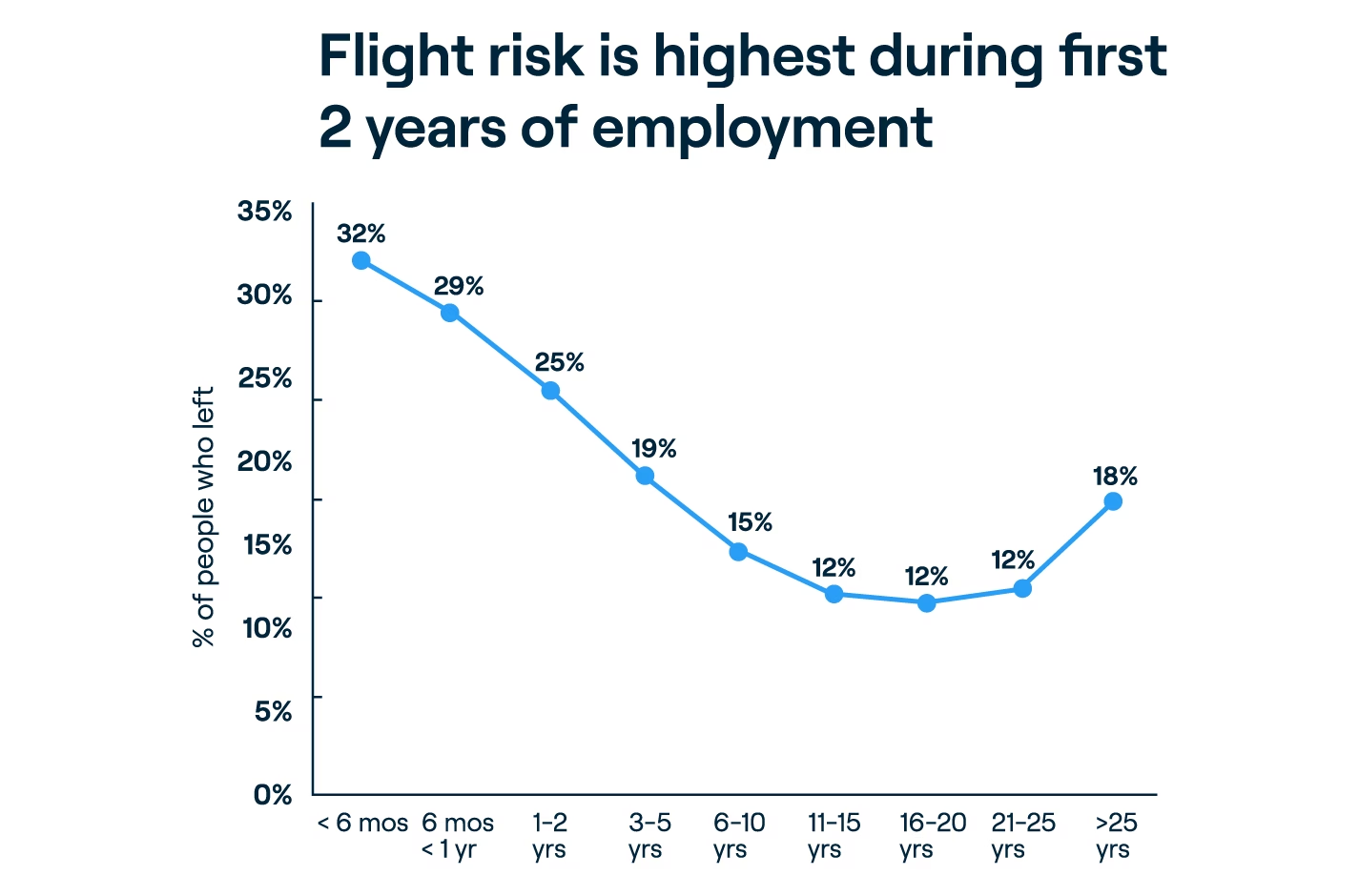
Additionally, at the role level, we see similar patterns for turnover to those we saw in engagement: greater turnover risk among certain front-line employees. The compounding effect of tenure on new front-line employees, who are already at greater risk for leaving, underscores the importance of onboarding efforts that extend well beyond orientation.
But encouragingly, strong leader-employee relationships reduce turnover risk: Teams with high leader index scores had an average turnover rate of 16% vs. teams with low leader index scores, which saw 23% of employees depart.


Analysis of survey results shows the critical impact of organizational culture on engagement and retention: In addition to a commitment to safety, equity, respect, and a sense of belonging are highly correlated with employee retention across all roles. And they have a well-understood link to safety outcomes: If staff members don’t feel respected, valued, and included, they are less inclined to speak up and raise concerns, putting patients and the organization at substantial risk.
Key driver analysis reveals nurses are more likely to stay with an organization when they feel a strong sense of inclusion and belonging and believe their job is the right fit for them. For physicians, feeling aligned with their organization—having respectful relationships with leadership, being part of decision-making processes, and sharing a common vision for the organization’s mission—plays a significant role in retention and engagement.
Our workforce engagement research reveals common approaches and practices among top performers. In addition to hardwiring the leadership behaviors that improve safety and reliability, top performers keep their fingers on the pulse of their workforce. They complement annual engagement surveys with an omnichannel, continuous listening strategy to allow for rapid surfacing of and response to pressing issues—helping to reduce friction and distractions experienced by staff to enable top-of-license practice and professional fulfillment.

Implications and opportunities
Attracting and retaining top talent is not a new priority for health systems. But the competitive labor market, coupled with a labor shortage that will persist into the future, mandates new approaches to the work. The healthcare workforce is under different pressures today than it was even just five years ago; employees’ needs and expectations have changed. Leading organizations are revamping their employee value proposition and talent management strategies in response.

Immediate work to address pressing needs
Leading health systems are focusing efforts on dual priority areas: meeting the immediate needs to retain, attract, support, and develop talent, and laying the groundwork to transition to and support care models of the future. Taking these actions is tantamount to making a down payment on building the social capital and trust organizations need to thrive in today’s challenging environment.
Onboarding: Modern onboarding programs recognize that building engagement starts on day one. Unlike orientation programs, robust onboarding programs focus on connecting new employees to the organization more broadly—its mission, vision, and values—to their unit or department, and, finally, to ongoing opportunities for their own professional development. Fostering a sense of belonging is key to success.
Front-line leader development: Nurse managers are the linchpins of inpatient acute care, but they often don’t get adequate training for the role. A standard, enterprise approach to leader development and coaching yields significant ROI, including higher nurse engagement, improved resilience among nurse managers, reduced nurse turnover, better clinical outcomes, and productivity.
Safety as a core value: Organizations that commit to zero harm and high reliability organizing (HRO) principles achieve gains in employee and patient safety—including psychological safety. In a period of transformation, leading health systems make it a priority to review, refresh, and recommit to enterprise behavior standards, as well as reconfirm mechanisms for accountability, learning, and improvement. They are paying close attention to safety culture, with a particular focus on violence and incivility experienced by caregivers.
Fix broken systems: A poor workforce experience is frequently due to inefficient systems and processes. Lasting solutions come from listening to front-line employees, whose direct experience provides essential insights. When these employees feel their voices are valued and understood, they’re more inclined to consistently offer useful feedback, fostering a positive feedback loop. To gather employee insights on a larger scale, top organizations are turning to innovative technologies, including AI-powered platforms, virtual focus groups, and crowdsourcing.
Future-proofing the workforce: The straightforward, but hard, work of cultural transformation
Change is constant in healthcare. And organizational culture ultimately determines which organizations weather the storm and emerge stronger following major change efforts. Culture is how values are expressed through formal elements of strategy, priorities, and policies, as well as through informal aspects of customs and behaviors. Organizations on the leading edge of the engagement curve have certain things in common across the formal and informal elements of culture. They are: an environment that fosters respect, inclusion, and safety; a commitment to consistently executing on best practices; and a willingness to redesign the work being done. These traits emerge in three principal areas:
1. Committed and involved senior leadership
Employees have confidence and trust in senior leadership. Senior leaders embody the organization’s mission and values in both word and deed—they lead the way with their own everyday behavior and actions. They are highly visible and clearly articulate the organization’s vision and strategy. They embrace transparency to build trust, foster accountability, and ensure a sense of belonging.

2. Established values and behavior standards
Employees feel the organization treats them respectfully. They also feel the organization seeks their feedback to pinpoint opportunities for improvement, as well as their input on just how to improve. Employees and physicians are aligned with senior leadership, and everyone is working toward the same goals. Importantly, there is accountability to abide by the organization’s values, and a method for remediation if people fall short.

3. Adopting high reliability organizing principles
HRO is usually thought of as an approach to achieving safe care and safe practice environments. But the true definition of HRO is “performing as intended consistently over time”—which is relevant in every aspect of care delivery. Adopting high reliability principles and practices can impact all performance domains—including workforce engagement and patient experience. The fundamental principles of HRO—which center around transparency, communication, expertise, and continuous learning and improvement—enable leaders to align mindsets and actions, reduce variation and barriers to great care, optimize processes, and empower people at every level of the organization.

The evolving expectations of today’s healthcare consumer
In 2023, Press Ganey national data revealed a consistent uptick in patients’ rating of experiences in acute inpatient care, almost completely reversing the downturn seen between 2020 and 2022. While patient experience in emergency departments continues to be a challenge for many healthcare systems, we’re beginning to see promising improvements in that area as well.
Leading health systems saw the benefit of offering flexible options for getting care during the pandemic—meeting demand by shifting volume to lower-intensity settings and modalities. Many have matured those COVID-stopgap measures, integrating them into their access strategies and establishing new access points for on-demand care via telehealth services and partnerships with retail providers and/or stand-alone urgent care providers.
Unlike acute care, medical practices sustained high performance, with “Likelihood to Recommend” (LTR) increasing during the pandemic. This reaffirms the patient-physician relationship as the cornerstone for care, which is an important consideration for evolving healthcare models and strategies. Establishing a trust-based relationship will always be a prerequisite for patient satisfaction and enduring loyalty.
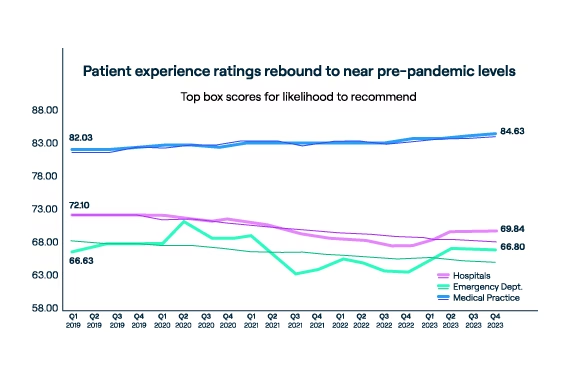
However, it’s clear that consumer expectations in healthcare are rapidly evolving. The convenience, simplicity, and personalized experiences enabled by technology in other aspects of our lives have led consumers to expect similar experiences in healthcare. This shift in consumer expectations is reflected in how people go about choosing a doctor.
A recent Press Ganey consumer survey reveals a growing trend among consumers to conduct online research when choosing a doctor, with 37% of respondents indicating they now find their doctors online. In fact, 2023 marked the first year the internet became more important for choosing a doctor than referrals from friends, family, or another physician. Moreover, consumers are consulting multiple websites and reading multiple reviews before choosing a doctor. Significantly, 84% of respondents stated they would not consider a physician rated less than 4 stars.
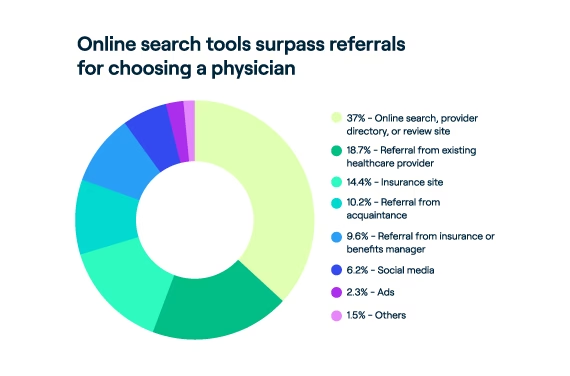
This shift in consumer behavior underscores the need for healthcare providers to adapt to meet new consumer expectations in healthcare by making performance ratings accessible, leveraging technology to enhance the patient experience, and focusing on earning and re-earning the trust and confidence of their patients with every encounter, across the full spectrum of encounters.
Drivers of patient trust and confidence
We see further evidence of evolving consumer expectations in healthcare when analyzing the impact of friction on patients’ willingness to recommend a medical practice. When a patient experiences friction at any time, it erodes their trust in their provider and the practice. Friction can occur before, during, or after care—in the form of challenges contacting the practice, getting an appointment, wait times, availability of lab results and other pertinent medical records, or receiving post-visit follow-up from the practice.
Patients who respond favorably to questions about these aspects of their care are highly likely to recommend the practice (99th percentile results). Conversely, any amount of friction erodes patients’ “Likelihood to Recommend”—and the magnitude of friction experienced has a corresponding negative effect on “Likelihood to Recommend”.
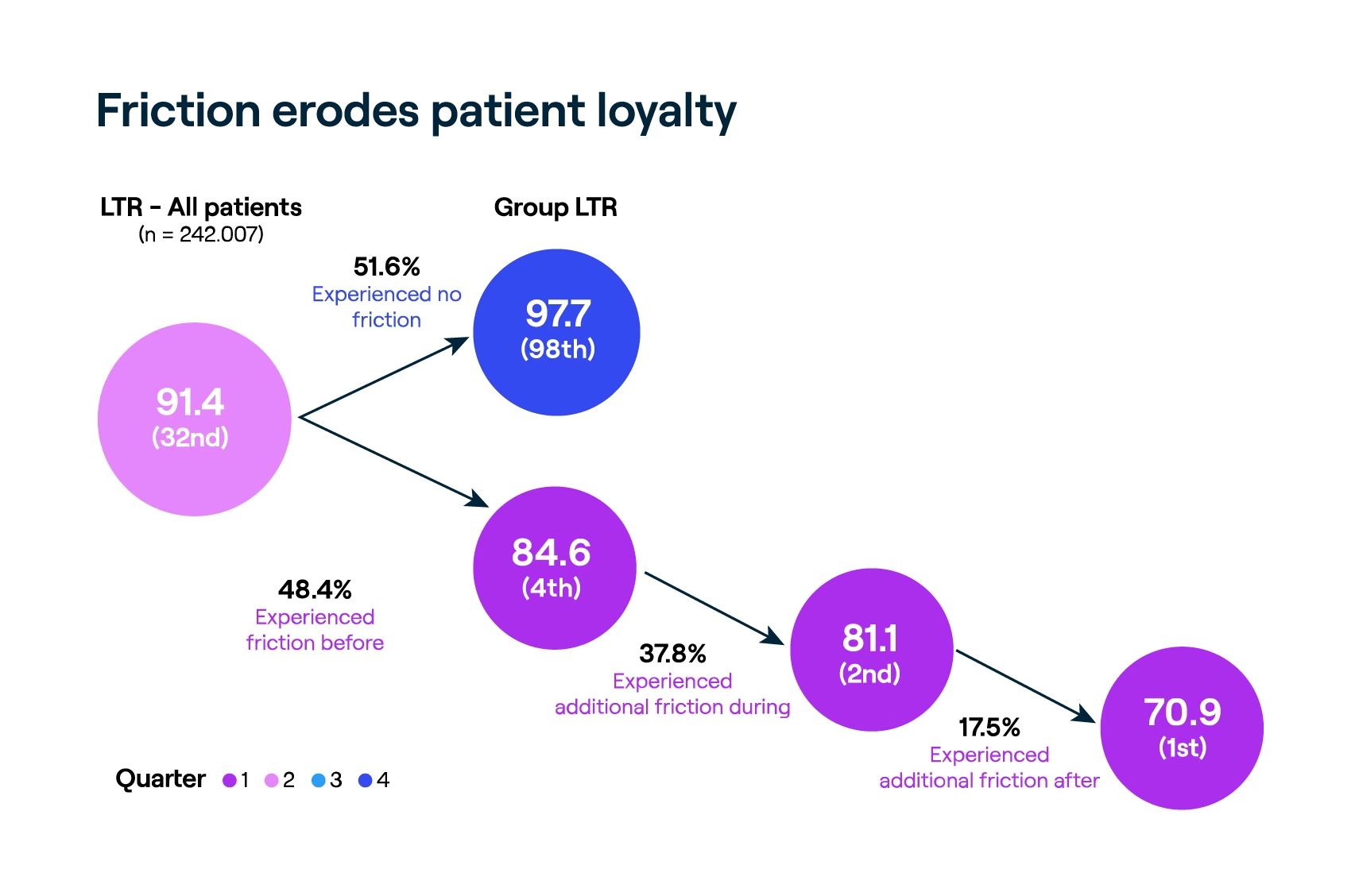
Clinicians often interpret low relative performance on patient experience scores as a critique of their bedside manner, yet the friction data reveals a different message: Suboptimal workflows and care processes torpedo the scores of even the most compassionate, skilled, and dedicated clinicians. Friction in the patients’ care journey erodes trust in the system and confidence in the medical practice. Eliminating friction and improving coordination builds trust with the medical practice and the care they provide.
Patients’ heightened awareness of safety
COVID taught patients to be alert to their safety in care environments, and we see the impact of patients’ perception of safety is showing up in their responses to the “Likelihood to Recommend” question. Our analysis of more than 12 million responses to ambulatory care surveys reveals that patients who give an unfavorable response to questions about whether staff provided care in a safe and secure manner are 2.5–3x less likely to recommend the hospital or medical practice.
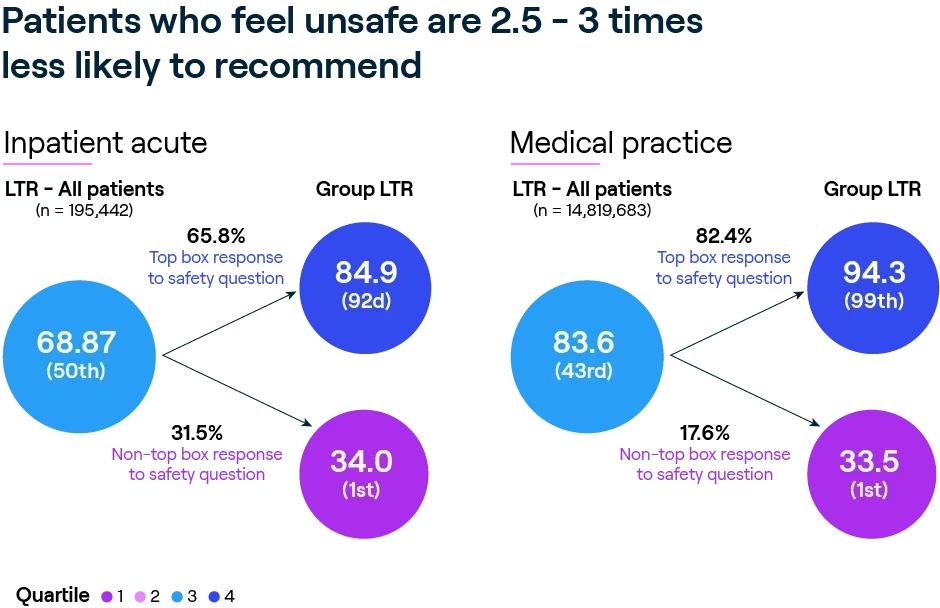
Consistent with contemporary definitions of harm, patients’ perception of safety extends beyond their physical safety to include interactions that contribute to emotional security or harm. Using natural language processing (NLP) to analyze survey comments, we find that patients describe experiences of feeling safe (or unsafe) in terms of feeling respected (or disrespected) in the way their caregiver communicated with them, through behaviors like how patiently next steps in the treatment are explained, being attentive to concerns, and giving thorough answers in a friendly manner to questions about safety.
Patient-provider interaction
Provider and staff interactions with patients do matter, especially in an environment where consumers have greater expectations and a heightened sensitivity to safety. Our analysis of 12 million patient responses to medical practice surveys shows that responses to questions on confidence in the provider’s skills, evidence of teamwork among members of the care team, demonstrated compassion for the patient (they are listened to; the provider demonstrates concern for their worries), and shared decision-making are powerful predictors of patients’ “Likelihood to Recommend” the practice. When care teams demonstrate all four attributes—providing care that inspires confidence, acting with coordination, and being visibly compassionate—99% of patients recommend the medical practice.
The loyalty impact of interactions between patients and the people involved in their care holds true across settings, with minor nuances. Regardless of where care is received, patients’ assessment of how they were treated—feeling respected, listened to, communicated with, included in decision-making—shapes their confidence in the system and the people caring for them.
Implications and opportunities

Rising consumer expectations in healthcare and the proliferation of new options for care adds imperative to accelerate care redesign. Health systems are leaning into this work, committing to finally and truly organizing around the needs of patients, with the goal of reducing complexity, tailoring care to the individual, and optimizing the patient experience.
The range of initiatives includes strengthening the digital front door, shifting more care to outpatient settings, partnering with other providers to improve access, establishing hospital-at-home services, investing in artificial intelligence (AI), and more.
Starting now, make healthcare easier
Reducing complexity where possible is key to building patient confidence and earning loyalty. Understanding where friction occurs in the patient’s journey is essential to solve the right problems. The work extends beyond traditional post-care surveys. To understand where the experience can be optimized, health systems need to gather feedback and input using dynamic and flexible methods. Leading systems are supplementing surveys with language analytics, digital focus groups, and electronic communities to really understand patient expectations and priorities.
Real-time, omnichannel listening
Continuous listening systems provide service recovery alerts to resolve individual issues and shine a light on system failures that require process redesign (e.g., wait times and poor care coordination) or service failures that indicate a need for training and coaching (e.g., communication skills and service behaviors). New capture modes, such as in-app or in-care feedback, and point-of-service QR codes complement traditional post-care surveys and identify additional sources of friction. Digital surveys designed specifically to measure the Human Effort Score sharpen focus and execution.
Artificial intelligence derived from NLP
Patient survey comments and other unstructured texts are a rich source of information, offering nuance to quantitative results. AI spots emerging themes that are difficult to replicate by human review, due to the sheer volume of comments. The results enable service recovery, offer healthcare consumer insights on the experience of new care models, and inform care redesign efforts.
Invite patient input at scale
Patients are often willing—and eager—to provide input to make care better, but health systems struggle to capture input representative of their full populations. New digital capabilities enable provider organizations to broaden their reach and invite input at scale. Virtual PX design sessions, digital patient panels, and digital communities open the aperture for input with synchronous and asynchronous models convenient and available to all members of the communities they serve.
Focus on the digital front door
High-performing organizations recognize that, today, the trust continuum begins online. In response, they bring diverse colleagues to the table to design the consumer experience (CX), reflecting an integrated CX/PX strategy. Together, the chief marketing officer, chief experience officer, and care delivery leadership are collaborating to ease the way for patients by focusing on key touchpoints and making relevant information available to consumers:
- Ensure provider directory information is complete and current to reduce friction.
- Publish patient experience ratings and comments in physician directories to aid research and decision-making, and to build trust through transparency.
- Publishing ratings and comments to third-party listings sites. Publishing to third-party sites offers the dual benefit of providing relevant information to consumers no matter where they research their options, while ensuring the information on those sites is derived from validated surveys and is representative.
Segment performance results to identify gaps
While best practices and high reliability principles offer the surest way to optimize the system, it remains essential to understand the unique needs of patients. There are important differences in how patients experience and evaluate care based on their health status, care needs, age, gender expression, and race or ethnic backgrounds. Leading health systems address variation by looking for it, then evaluating whether best practices or friction have an equal impact for all groups.
- Segment patient experience results by patient attributes—both quantitative results and AI analysis of unstructured text.
- Use key driver analysis to determine if key drivers are equally impacting all groups.
- Invite input from groups experiencing gaps using digital and virtual engagement modes, such as virtual PX design sessions and digital patient panels.
Leverage HRO practices

HRO principles and practices are routinely thought of as foundations for safety and quality, but not routinely considered as the basis for consistently excellent experience of care. In studying organizations that have performed in the 90th percentile consistently for two years, three high reliability practices emerge.
- Established behavior standards: These are articulated and modeled at every level in the organization. In many cases, these standards have evolved from first-generation service behaviors (e.g., walking patients to their destination, eye contact) to universal relationship and reliability skills that promote patient and colleague relationships.
- Promote teaming through daily huddles: The practice of team huddles in both clinical and nonclinical areas improves the employee experience and is foundational to consistently delivering a coordinated team experience to achieve optimal outcomes and experience.
- Structured leader rounding initiatives: These include rounding on both patients and caregivers. Rounding initiatives ensure that leaders have the structure and process to connect consistently with patients and their teams. Rounding provides routine opportunities to model behaviors, give positive feedback and provide coaching, and demonstrate leaders’ commitment to promoting safe, high-quality, compassionate care—as well as engaging caregivers to deliver that care.
Future-proofing the patient journey: The patient experience, care innovation, and high reliability organizing
Increasingly complex care is moving outside the walls of hospitals, allowing for excellent clinical outcomes in a more personalized, compassionate, and convenient way. Leading organizations are focused on innovating and rapidly iterating toward minimally disruptive medicine—care pathways that reduce the suffering of patients, simplify the journey, and facilitate coordination among providers and caregivers. Moving quickly to integrate innovations into daily work, once they are proven to meet their objectives, is key. When it comes to innovating effectively and safely, then translating innovation pilots into practice, HRO competencies act as an accelerant.
Organizations that have adopted HRO principles will recognize how they serve as a chassis for innovation. Transformation through organizational learning is at the heart of HRO. In studying Press Ganey client performance before, during, and following the pandemic, we observed that organizations that fully embrace HRO principles and practices were more resilient across all performance domains to both the initial and trailing effects of COVID. Hardwired HRO competencies enabled them to respond more rapidly through reliability-based learning, adaptation, and innovation.
On top of committing to best practices, HRO involves wrapping around those best practices the competencies that ensure ongoing organizational learning and best practices sustainment—essential elements for improvement and transformation. The very same skills that help organizations reduce variation and improve outcomes serve as a disciplined process and framework for intelligent risk-taking—exploring and trying new ideas that enable transformation.
The essential people competencies of HRO
HRO principles reduce variation and spur innovation*
- Sensitivity to operations: Understanding that front-line staff members are best positioned to identify opportunities for improvement and the ways to address them. Routinely incorporating their input into design. Leveraging operating data to fuel understanding and expose gaps.
- Deference to expertise: Putting knowledge above authority and encouraging all people to speak up when they notice a problem or have an idea that could eliminate friction and lead to improvement.
- Reluctance to simplify: A commitment and discipline to seek full explanations of complex situations instead of relying on superficial understanding.
- Preoccupation with failure: Thinking through all possible sources of harm and scenarios where it could occur, or that might cause the objective to be missed. Spotting and responding to failure quickly when it does occur.
- Commitment to resilience: Rapidly assessing and responding to challenges to achieve recovery.
Parting thoughts: The role of social capital in transformation
Working harder will not be enough to address the issues facing healthcare organizations. And whatever improvements can be achieved by “tightening belts” have likely already been realized. We are at a critical juncture, where organizations must change how they work to deliver care and improve quality, safety, and the Human Experience for all their stakeholders. Focusing on building social capital will be an essential component of success.
Given the nature of the challenges healthcare organizations face, social capital is at least as important as financial capital—maybe more so, since funds can be obtained from outside sources. Only an organization’s leaders and managers can foster teamwork, cultures of respect, trust, and high reliability—the essential attributes for mobilizing teams and engaging people in the work of transformation. We know change happens at the speed of trust; we see social capital as fuel in the engine to propel us into the future.
The insight that has emerged through our interactions with many organizations—especially consistently high-performing systems—is this: Just as organizations have strategies for managing financial capital and human capital, they need a strategy for managing social capital. They need to measure it and ensure their leaders understand how to build it and be good stewards of it. Every manager must function like the CFO of social capital for their team, and approach it with the same intensity and discipline that an actual CFO applies to fiscal resources. We know change is coming. Social capital can help us ensure the change that happens is the change we want to see.