
Elevate your event reporting to drive high reliability
Eliminate harm before it occurs
Our High Reliability Platform (HRP) simplifies safety event reporting. See where errors occur, understand the causes, and fix things so that they don’t happen again. And our Patient Safety Organization (PSO) is a confidential space where you can share safety events and best practice with peers.
Get to the root cause of harm
Safety won’t wait
Our high reliability platform is ready to go on day one to immediately kick off your ability to report events, including complaints and grievances-not weeks or months down the line. Start using our forms, dashboards, and analytics out of the box, then customize from there.
Shareable insights at your fingertips
No complex tech training needed. Your team can collaborate and share insights, conduct root cause analysis, and identify trends to prioritize instantly with our flexible and easy-to-use dashboards.
Safety, across the board
The HRP platform engages your whole team in highly reliable safety event reporting and resolution. Reporting concerns on the move is super simple too, with a SMART Reporter App embedded directly in your patient charts.
Promote clarity and collaboration
Safety can be compromised when employees are afraid of the blame game. Tools within our risk event reporting system include real-time alerts, action plans, and dashboards, all of which break down silos and make transparency the norm.
HPI PRESS GANEY PSO
Supercharge your path to zero harm
A safe space to collaborate and share. Our Patient Safety Organization (PSO) is officially listed with the Agency for Healthcare Research and Quality (AHRQ). It’s a legally protected, confidential forum for sharing insights on patient safety.
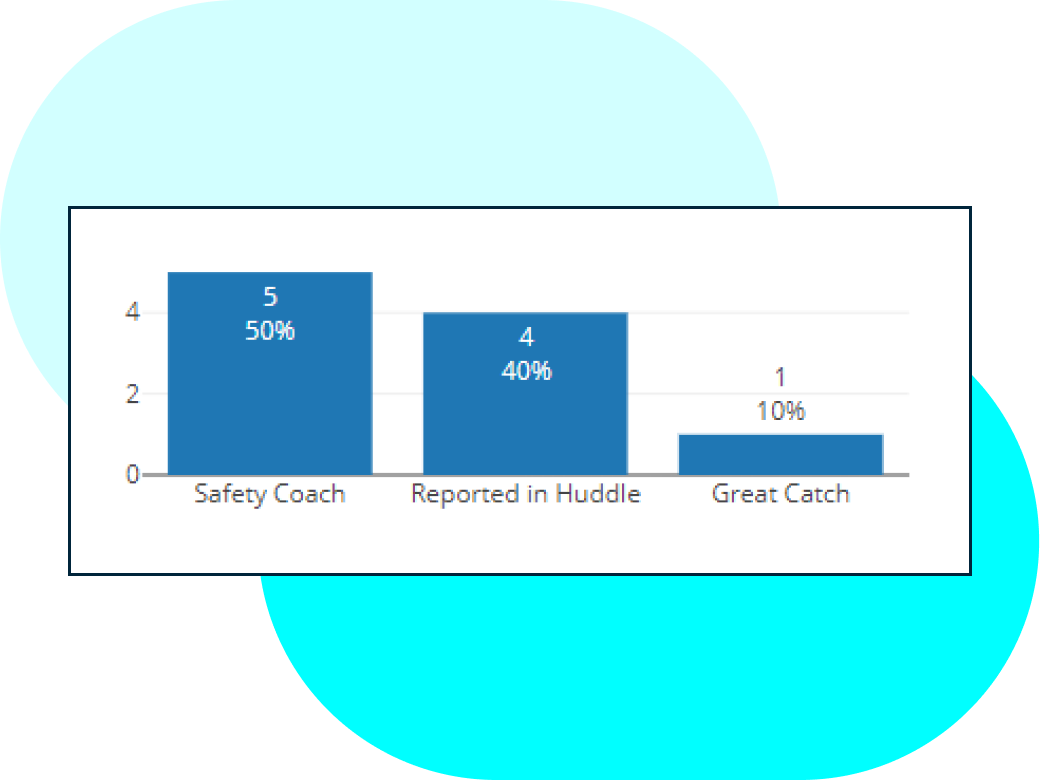

SAFETY EVENT reporting
Stop harm in its tracks
Our healthcare incident reporting system, our patient safety organization, and our commitment to making zero harm a reality are the foundation of how we are supporting your safety goals.
best practices and high reliability
Supercharge your path to zero harm
Zero harm is closer than ever before, and we’re doing our part to make it a reality. We work closely with healthcare leaders to stop patient and employee harm before it happens, through proven best practices and high reliability organizing (HRO).

Giving you the tools to make a difference
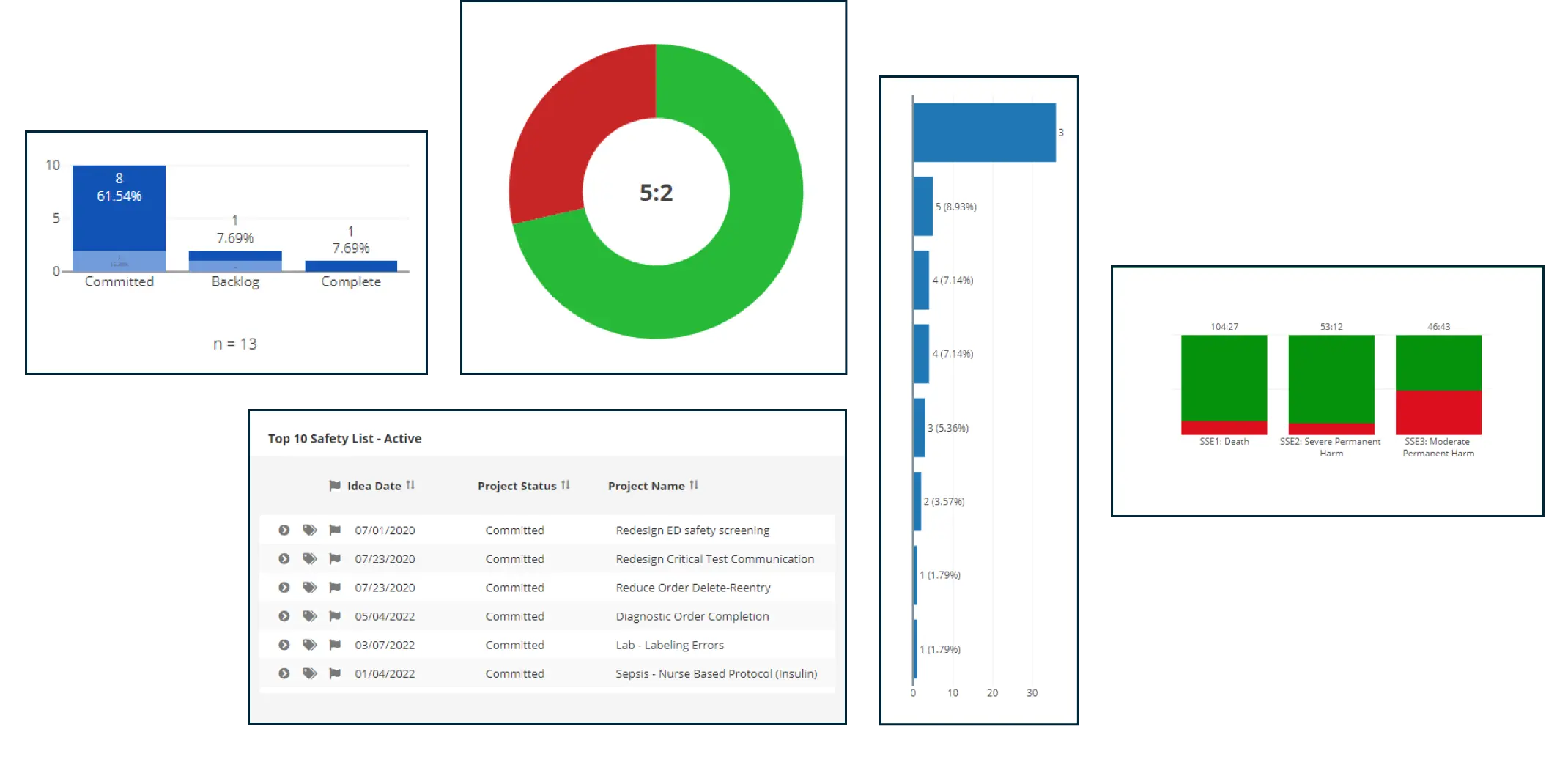
Your biggest challenges meet our best solutions
problems we solve
Patient & workforce safety
consulting
Safety & high reliability
Your role
Safety & quality leader
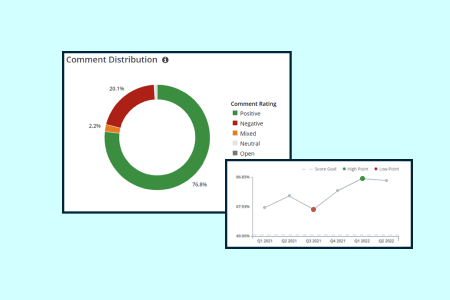
industry initiative
Safety 2025
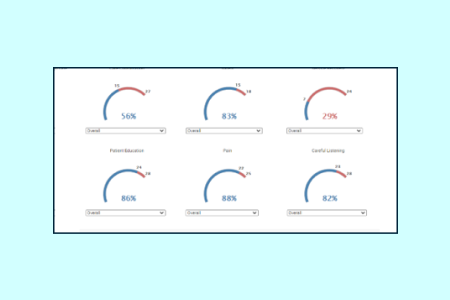

“Our improvement is not a siloed approach—we share similar teams; we share similar conversations. And high reliability is the foundation of it all.”
Paul Lambrecht
Vice President of Quality and Patient Safety, Inspira Health Network
High reliability & PSO
Level up your safety strategies
Get in touch, and we’ll take you on a tour of our safety solutions.
